Anal warts usually are caused by HPV. HPV is a virus and the warts are the outcome. However, remember that not every growth in the anal area is an anal wart caused by HPV.
It must be diagnosed by your medical doctor only. HPV is very common in sexually active men and women and can sometimes have serious health consequences. About 20 million Americans are currently infected, and about 5.5 million people become newly infected each year.
The virus can infect the Anal genital skin and the linings of the vagina, cervix, rectum, and urethra. They come in different shapes and color. Typically they present a cauliflower like growth scattered around randomly, however, it might take on different looks that could mimic other skin presentation. For Example: they could look like mole, skin tag, cyst, keratosis, etc.
They come in different shape such as raised, flat, big and small. Many patients have these growth for months and years and they might not even know it. This becomes alarming when patients see multiple lesions and start thinking that they are facing ongoing and spreading disease before seeking medical attention. Many lesions in the anal area could be easily mistaken by anal warts.
I always tell my patients; untreated genital warts have a big chance of infecting the anal area. I have seen so many heterosexual patients in my practice over years with anal warts and almost every single time, patients point out the following concern:
You don't have to have anal intercourse, although, anal intercourse increases your chance of infection. Regarding the female anatomy; the vaginal opening is in close proximity to the anus, so the male genital area could be in contact with the perianal area during intercourse.
Unfortunately, the treatment of anal warts is much more difficult than genital warts. They are more stubborn due to anal anatomy and physiology. Many routine treatment routes cannot be used in the anus which could lead to significant discomfort and complications such as as topical acid application, etc. In many cases anal warts need to be treated in a hospital setting, so it is imperative for patients to seek care as soon as getting infected with one before it's too late.
Needless to say, it is imperative to treat your genital warts before they extend to the anal area. Anal warts create more complications and symptoms than genital warts and it is harder to treat them and some of which listed as follow:
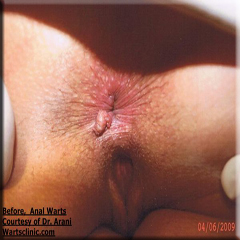
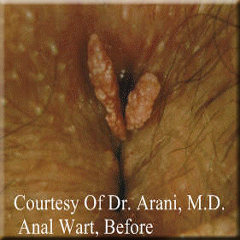
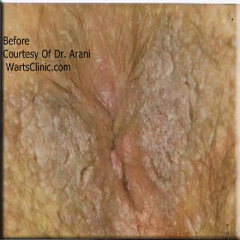
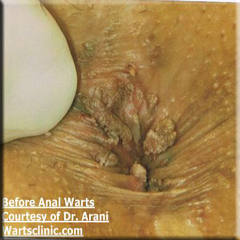
Treatment of anal warts should be complete. It means you should not have any wart left behind when removal procedure is finished.
After you have completed your treatment, you should go back to your doctor periodically (depending on your doctor's decision) for re-evaluation to check if there are any new warts, which should be immediately eradicated.
Human Papilloma Virus can cause cancer, however the location of infection plays important role of getting cancer or not.
HPV could cause cancer on penile but is not as common as causing anal cancer. In other words, you have a much higher chance to get anal cancer than penile cancer by HPV. It is imperative that your physician keep that in mind when treating anal HPV.
CIN is usually caused by HPV 16, 18, 31, 33, or 35. It is occasionally found in visible genital warts and has been associated with external genital squamous cell carcinoma in situ (cancer), bowenoid papulosis, Erythroplasia of Queyrat, and Bowen’s disease of the genitalia. These variants of HPV also have been associated with vaginal, anal, anogenital, and some head and neck squamous cell carcinomas.
An anal Pap smear is similar to a vaginal/cervical pap smear and tests for abnormal changes in the cells of the anus.
It is an important procedure often recommended to the patient with anal HPV to detect cancerous or precancerous changes.
Any suspicious lesions found by physical examination should be biopsied and sent to a laboratory for evaluation by a pathologist (a physician who evaluates tissue samples under a microscope). Any cancer or other abnormalities are then reported to the physician who performed the biopsy.